When people ask what sciatica is, they are usually trying to understand a very specific kind of pain: pain that starts in the lower back or buttock and travels down the leg in a nerve-like pattern. Sciatica is not a disease on its own. It is a symptom pattern caused by irritation or compression of the nerves that form the sciatic nerve pathway, most often in the lower spine.
This type of pain is often different from ordinary back pain. Patients may describe it as sharp, shooting, burning, or electric. It may travel below the knee and into the calf or foot, and it can come with numbness, tingling, or weakness. In many cases, sciatica improves with time and conservative care, but some cases need medical assessment and, in selected situations, imaging.
For patients seeking answers in a radiology center in Kuwait, one important point is this: imaging is not automatically needed for every episode of sciatica. In uncomplicated cases, early scans often do not change first-line treatment. But when symptoms are persistent, worsening, or linked to red flags, imaging such as MRI in Kuwait or sometimes CT scan in Kuwait may help identify the cause and guide the next step in medical care.
What is sciatica?
Sciatica refers to pain caused by irritation or compression of a lumbar or sacral nerve root that contributes to the sciatic nerve. Even though people often say “the sciatic nerve is trapped,” the problem commonly begins higher up in the lower spine, near the nerve roots, rather than in the leg itself. That is why some medical sources describe sciatica as a form of lumbar radiculopathy.
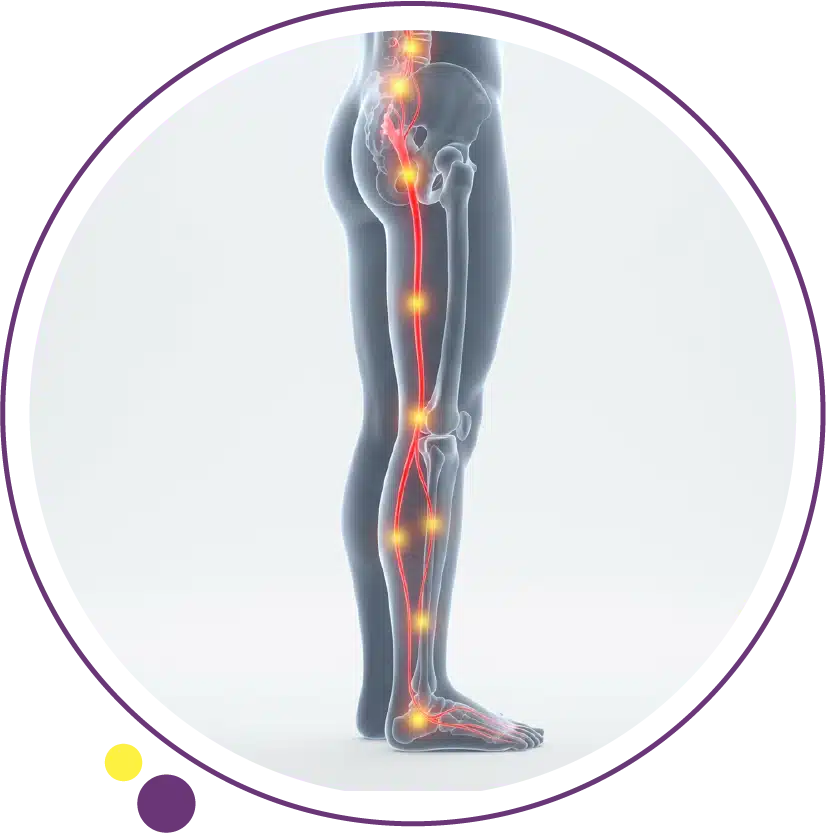
The sciatic nerve pathway runs from the lower back through the buttock and down the leg, so symptoms can be felt anywhere along that route. A person may have pain mainly in the buttock and thigh, while another may feel pain, tingling, or numbness all the way to the foot. This variation depends on which nerve root is affected and how much irritation is present.
Sciatica usually affects one side. It may come with lower back pain, but often the leg pain is more noticeable than the back pain itself. That is a useful clue because muscle-based low back pain often stays more localized, while nerve pain tends to travel.
What causes sciatica?
The most common causes of sciatica are conditions that put pressure on the lumbar nerve roots. Sciatica most often happens when a herniated disc or an overgrowth of bone puts pressure on these nerve roots. Other common causes include spinal stenosis, spondylolisthesis, and back injury.
A herniated disc is one of the best-known causes. The soft center of a spinal disc can bulge or push outward and irritate a nearby nerve root. When that happens, the pain is not limited to the spine. It can travel down the leg and produce the typical sciatica pattern.
Another common cause is spinal stenosis, which means narrowing of spaces in the spine where nerves pass. As those spaces narrow, nerves can become compressed, producing pain, tingling, or weakness in the leg. Spondylolisthesis, where one spinal bone slips out of place relative to another, can also contribute.
Less commonly, other structural problems such as trauma, tumors, infection, or severe inflammatory change may irritate or compress the nerve roots. That is one reason doctors pay close attention to severe or unusual symptoms rather than assuming every case is a simple disc problem.
What does sciatica feel like?
Patients often ask this because they want to know if their pain sounds like nerve pain or something else. Classic sciatica pain often feels sharp, burning, stabbing, or electric. Some people describe it as a sudden jolt down the leg. Others notice a constant deep ache with intermittent shooting pain.
The pain may worsen when sitting for a long time, coughing, sneezing, or straining. These actions can increase pressure around an irritated nerve root and temporarily intensify symptoms. The discomfort may also be worse with certain movements or positions.
Sciatica can also include non-pain symptoms. Tingling, numbness, “pins and needles,” heaviness, or weakness in part of the leg or foot are all possible. Some people notice reduced feeling in the feet. Others feel that the leg is not as strong or reliable as usual.
What are the main symptoms that suggest sciatica?
Several symptoms together make sciatica more likely than simple back strain. The most helpful pattern includes:
- pain that starts in the lower back or buttock and runs down one leg
- pain that travels below the knee
- burning, shooting, or electric pain
- tingling or numbness in the calf, foot, or toes
- weakness in the leg or foot
- symptoms that worsen with sitting, coughing, or sneezing
Not every patient has every symptom. Some mainly have pain. Others have more numbness or tingling than pain. What matters most is the nerve-pattern distribution and the association with lower spine symptoms or provocation.
Why would a doctor think it is sciatica and not another cause of leg pain?
Doctors do not diagnose sciatica from one symptom alone. They look at the pattern. Pain that clearly follows a nerve distribution from the back or buttock into one leg is more suggestive of sciatica than pain isolated to the knee, calf, or hip. Associated numbness, tingling, or weakness also increases suspicion of nerve-root irritation.
At the same time, many other conditions can mimic sciatica. Hip disorders, muscle injury, peripheral nerve problems, vascular disease, and other spinal problems can all cause leg pain. That is why clinicians combine symptom history with a physical examination rather than relying on symptoms alone.
When should you see a doctor for sciatica?
You should seek medical review if the pain is severe, not improving after a period of self-care, or interfering with sleep, walking, work, or normal daily activities. You should also seek care if home treatment is not helping, the pain is worsening, or symptoms keep returning.
It is also reasonable to seek earlier evaluation if you notice numbness, tingling, or weakness becoming more noticeable, even if you do not have emergency symptoms. Persistent or progressive nerve symptoms may need a more formal diagnosis and a structured treatment plan.
Which symptoms are red flags?
Most sciatica is painful but not dangerous. However, some symptoms may suggest severe nerve compression or another urgent spinal problem. Urgent emergency evaluation is needed if sciatica affects both sides, if there is severe or worsening weakness or numbness in both legs, if there is numbness around the genitals or anus, or if there is difficulty starting urination, loss of bladder control, or loss of bowel control.
These symptoms can point to cauda equina syndrome, a spinal emergency. Patients should not wait for a routine clinic visit if these features appear. Sudden major neurologic change also deserves urgent assessment.
How is sciatica diagnosed?
Diagnosis usually starts with the medical history and physical examination. A clinician asks where the pain starts, where it travels, what makes it worse, whether numbness or weakness is present, and how long the symptoms have been going on. The physical exam may include checking strength, sensation, reflexes, and movements that stretch the nerve roots.
This first step is often enough to strongly suspect sciatica. Additional testing is more likely when symptoms are prolonged, unusually severe, progressive, or difficult to explain. Imaging and tests such as electromyography may be used in selected cases.
When is imaging needed for sciatica?
This is one of the most important questions for patients. Imaging is not usually recommended early for uncomplicated low back pain with or without sciatica in non-specialist care unless serious pathology is suspected. Routine early imaging may not change initial management and can show common age-related findings that are not actually causing the symptoms.
Imaging becomes more useful when symptoms are persistent despite treatment, when the patient may be a candidate for procedures or surgery, or when red flags suggest serious compression, infection, tumor, fracture, or another important underlying cause. In those situations, imaging can help identify the structural reason for the nerve pain.
Is MRI or CT better for sciatica?
For many patients with persistent or complicated sciatica, MRI is the preferred imaging test because it shows soft tissues well, including discs, nerve roots, ligaments, and spinal canal narrowing. MRI helps evaluate disc and joint disease and compression or inflammation of nerves, all of which are relevant to sciatica.
CT Scan can still be helpful in selected situations, especially when MRI is not suitable, when bony detail is important, or in special studies such as CT myelography. Spine CT is also useful in trauma because it is fast and accurate. The appropriate choice depends on the clinical question and the patient’s situation.
For patients in a medical imaging center in Kuwait, that means the “best” scan is not the same for everyone. The best scan is the one that answers the doctor’s question most clearly and safely.
What should patients expect during imaging?
If your doctor requests MRI in Kuwait, the exam is usually painless and does not use ionizing radiation. You lie still on a table while the scanner creates detailed images of the lumbar spine. MRI is especially useful because it shows discs and nerve roots clearly. Patients should mention implants, pacemakers, pregnancy, kidney issues, or severe claustrophobia before the scan.
If CT scan in Kuwait is chosen, the exam is also quick and painless. Spine CT is often used to assess spinal column damage, especially in injured patients, and may be used when MRI is not suitable. Depending on the reason for the scan, special preparation may or may not be needed.
What simple self-care helps sciatica?
For many people, sciatica responds to conservative care. Resting for a day or so may help, but staying inactive usually makes symptoms worse. Gentle movement, staying active, and trying exercises and stretches are usually more helpful than prolonged bed rest.
Gentle movement, pacing activity, avoiding long periods of sitting, and gradually returning to normal function are usually sensible first steps. Some patients also find relief with heat or cold packs and guided physical therapy exercises. The goal is to stay mobile without forcing movements that sharply worsen symptoms.
Are there limitations or precautions patients should know about?
Yes. One important limitation is that imaging findings do not always match symptoms perfectly. Common changes such as disc bulges or age-related degeneration may appear on scans even in people without pain. That is why imaging results must be interpreted in the full clinical context, not as the whole diagnosis by themselves.
Another important point is that not all nerve pain down the leg is identical. Some symptoms that feel like sciatica may come from other nerve, muscle, joint, or vascular problems. This is why a good examination remains essential even when imaging is eventually ordered.
Frequently asked questions
- Is sciatica a condition or a symptom?
Sciatica is best understood as a symptom pattern rather than a single disease. It describes nerve-related pain and other symptoms that travel down the leg, usually because of irritation or compression of lower spinal nerve roots.
- Is sciatica always caused by a slipped disc?
No. A herniated or slipped disc is a common cause, but it is not the only one. Spinal stenosis, spondylolisthesis, bone overgrowth, and back injury can also cause sciatica.
Do all people with sciatica need an MRI?
No. Routine early imaging is not usually needed for uncomplicated sciatica. MRI becomes more relevant when symptoms are persistent, worsening, associated with red flags, or likely to change management.
Can sciatica improve without surgery?
Yes. Many cases improve with time, activity modification, self-care, and conservative treatment. Surgery is usually considered only in selected cases, especially when symptoms are severe, prolonged, or associated with worsening weakness or emergency red flags.
What symptom is most concerning in sciatica?
The most concerning symptoms are saddle numbness, loss of bladder or bowel control, severe or worsening weakness, and symptoms affecting both legs. These need urgent medical assessment because they may indicate severe nerve compression.
Is walking good for sciatica?
In many cases, yes. Gentle activity and avoiding prolonged inactivity are usually advised because staying still often makes symptoms worse. The activity still needs to be paced according to symptom severity.
Your diagnostic journey at Images for Health
Understanding what sciatica is helps patients recognize the difference between ordinary back pain and nerve-root pain that may need closer attention. Early evaluation and timely imaging, when clinically indicated, can help doctors identify disc problems, spinal narrowing, or other causes behind persistent or progressive symptoms. Accurate radiology supports better clinical decision-making, especially when symptoms are prolonged, worsening, or linked to red flags. In a specialized medical imaging center in Kuwait, patient comfort, safety screening, and high-quality imaging all help improve diagnostic clarity and follow-up planning.
Core services available at Images Diagnostic Center in Kuwait include:
Patients may Contact the center for more information or to arrange an appointment when imaging has been recommended. Images for Health supports trusted radiology services and advanced diagnostic imaging in Kuwait, with a focus on diagnostic quality, patient-centered care, and reliable imaging support for spine, nerve, and musculoskeletal evaluation.