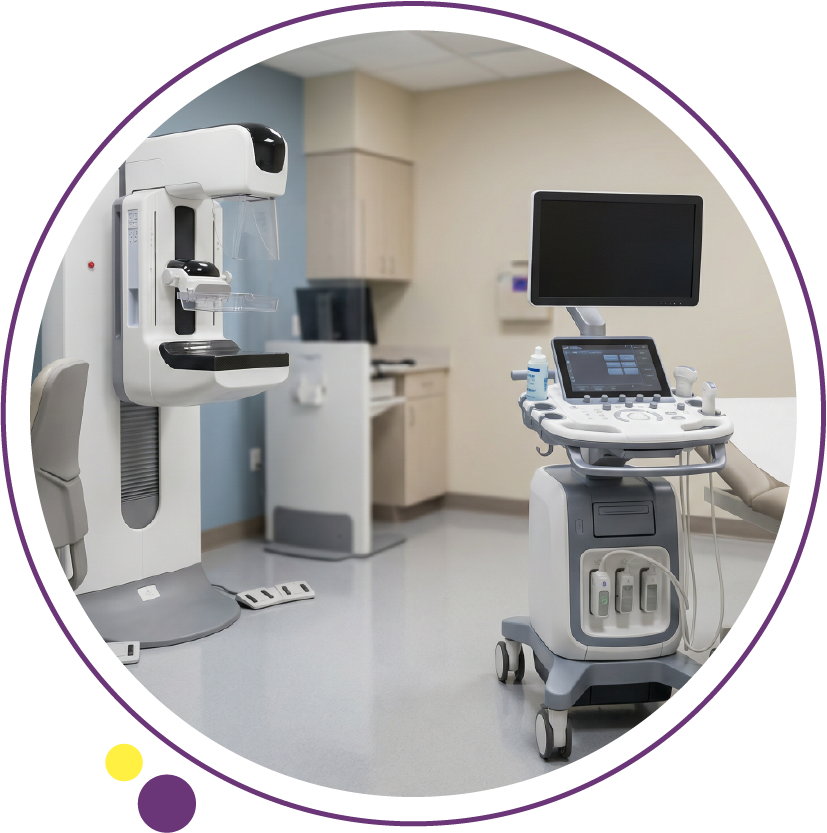
When comparing mammogram vs ultrasound, the question is rarely which test is “better” in general. The clinically correct question is which modality is more appropriate for a specific patient, age group, breast density, symptom profile, and screening objective. At Images Diagnostic Center in Kuwait, breast imaging protocols are structured around clinical indication, breast composition, and international reporting standards to ensure diagnostic clarity and safety.
Breast imaging is not interchangeable. Mammogram Kuwait services and ultrasound in Kuwait examinations serve different but complementary roles. Understanding when each test is indicated helps patients make informed decisions and supports referring clinicians in selecting the most appropriate imaging pathway.
How does a mammogram work and what does it detect?
A mammogram uses low-dose X-ray technology to evaluate breast tissue for early signs of malignancy, including microcalcifications, architectural distortion, and masses that may not be palpable.
Technical overview
- Uses ionizing radiation at optimized low doses
- Standard views include craniocaudal and mediolateral oblique projections
- Compression spreads breast tissue to reduce overlap and improve resolution
- Digital systems allow image manipulation for enhanced detection
According to ACR practice parameters, mammography remains the gold standard for breast cancer screening in women over 40, particularly for detecting calcifications that may indicate ductal carcinoma in situ.
Clinical indications for mammography
- Routine breast cancer screening beginning at age 40
- Follow-up of prior abnormal imaging
- Evaluation of microcalcifications
- Monitoring after breast-conserving surgery
- Surveillance in high-risk patients
Mammography is particularly valuable for detecting early non-palpable cancers, which may not produce symptoms.
How does breast ultrasound differ from mammography?
Ultrasound uses high-frequency sound waves rather than radiation. It is frequently used as an adjunct to mammography or as a primary tool in specific age groups.
Technical principles
- Real-time imaging
- No ionizing radiation
- Excellent soft tissue characterization
- Useful for differentiating cystic versus solid masses
Breast ultrasound provides detailed assessment of lesion margins, internal vascularity using Doppler ultrasound, and guidance for biopsies.
Clinical indications for ultrasound
- Evaluation of a palpable lump in women under 40
- Assessment of dense breast tissue
- Clarifying indeterminate findings on mammography
- Evaluating breast pain or localized swelling
- Image guidance for core needle biopsy
Ultrasound excels in evaluating symptomatic patients and dense breasts, where mammographic sensitivity may be reduced.
What makes mammogram vs ultrasound different in diagnostic accuracy?
Diagnostic accuracy depends heavily on age, breast density, and clinical scenario.
Mammography accuracy
- High sensitivity in fatty breasts
- Superior detection of microcalcifications
- Screening tool validated by decades of outcome data
Ultrasound accuracy
- Higher sensitivity in dense breasts
- Better for distinguishing solid versus cystic masses
- No radiation exposure
In women with dense breast tissue, mammography sensitivity may decrease due to tissue overlap. Supplemental ultrasound can increase cancer detection rates in selected patients.
However, ultrasound alone is not a substitute for screening mammography in women over 40 unless clinically indicated.
What makes 3D mammography more sensitive in certain patients?
Digital breast tomosynthesis, often called 3D mammography, captures multiple thin-slice images through the breast, reducing tissue overlap.
This technique improves:
- Lesion visibility
- Detection in dense breasts
- Reduction of recall rates
Tomosynthesis enhances diagnostic confidence, especially in women with heterogeneously dense tissue.
When is ultrasound preferred over mammography?
Ultrasound is typically the first-line imaging modality in:
- Women under 30 with a breast lump
- Pregnant or lactating patients
- Patients with focal breast pain
- Evaluation of axillary lymph nodes
In these scenarios, radiation avoidance and superior soft tissue differentiation make ultrasound clinically appropriate.
For women between 30 and 40 with symptoms, combined imaging may be recommended depending on risk factors.
Patient preparation: what should you know before your visit?
For mammography
- Avoid deodorant or talcum powder on the day of exam
- Schedule one week after menstrual cycle when possible
- Inform staff of pregnancy or implants
- Bring previous imaging studies for comparison
For breast ultrasound
- No fasting required
- Wear two-piece clothing for comfort
- Inform staff of prior biopsies or surgeries
Proper preparation reduces repeat imaging and improves diagnostic quality.
Step-by-step patient journey at Images Diagnostic Center
Breast imaging at Images Diagnostic Center follows a structured workflow aligned with international best practices.
1. Arrival and registration
Patient identification and prior imaging review.
2. Clinical screening
- Symptom assessment
- Risk factor evaluation
- Pregnancy screening if applicable
3. Imaging acquisition
For mammography:
- Technologist positions breast carefully
- Compression applied briefly for image clarity
For ultrasound:
- Sonographer performs systematic quadrant scanning
- Doppler ultrasound used when vascular assessment is needed
4. Image interpretation
Radiologists review images using standardized BI-RADS classification to ensure consistent reporting.
5. Report delivery
Structured reporting supports clear communication with referring physicians.
How fast can a breast imaging report be ready?
Radiology report turnaround time depends on:
- Complexity of findings
- Need for comparison with prior studies
- Requirement for additional views
At a structured accurate diagnosis imaging center in Kuwait, workflow protocols prioritize timely reporting without compromising thorough review.
Same-day preliminary assessments may be possible in selected cases, especially when additional views are required during the same visit.
Contrast media in breast imaging: when is it used?
Contrast agents are not used in routine mammography or ultrasound. However, contrast-enhanced MRI may be recommended in high-risk screening or staging.
Precautions include:
- Renal function assessment
- Allergy history screening
- Pregnancy considerations
Contrast-enhanced breast MRI provides superior soft tissue contrast and is indicated for specific clinical scenarios.
Breast density and its impact on imaging choice
Breast density is categorized into four groups based on BI-RADS criteria.
Dense tissue:
- Appears white on mammogram
- Can obscure small tumors
- May reduce sensitivity of standard mammography
Supplemental ultrasound or MRI may be recommended for selected patients with dense breasts and elevated risk.
Radiation safety and dose optimization
Mammography uses low-dose radiation consistent with ACR dose optimization standards.
Dose considerations include:
- Age and indication
- Avoiding unnecessary repeat exposures
- Quality control calibration
Ultrasound involves no ionizing radiation and is safe in pregnancy.
Images Diagnostic Center adheres to established radiation safety principles to ensure patient protection.
Biopsy guidance and follow-up pathways
If imaging reveals a suspicious lesion:
- Ultrasound-guided biopsy may be performed
- Stereotactic guidance may be used for calcifications
Post-biopsy care instructions typically include:
- Avoid strenuous activity for 24 hours
- Monitor for swelling or bruising
- Follow pathology consultation schedule
Structured follow-up ensures coordinated care.
Choosing between mammogram vs ultrasound for screening
Screening recommendations generally include:
- Annual or biennial mammography starting at age 40
- Earlier screening for high-risk patients
- Ultrasound as supplemental tool, not replacement
Clinical decision-making is individualized.
FAQs
- Is mammogram more accurate than ultrasound?
Mammography is more accurate for detecting microcalcifications and early asymptomatic cancers in women over 40. Ultrasound is more sensitive in dense breast tissue and better at evaluating palpable lumps.
- Can ultrasound replace a mammogram?
Ultrasound does not replace screening mammography in most women over 40. It complements mammography in dense breasts or when symptoms are present.
- Does mammography hurt?
Compression may cause temporary discomfort lasting a few seconds. It improves image clarity and reduces radiation dose.
- Is ultrasound safer because it has no radiation?
Ultrasound involves no ionizing radiation and is safe in pregnancy. However, safety alone does not determine which test is clinically appropriate.
- How often should I get screened?
Screening frequency depends on age, risk factors, and physician recommendation. Most average-risk women begin regular mammography at age 40.
Informed imaging decisions for better outcomes
Selecting between mammogram and ultrasound depends on clinical indication, breast density, age, and symptom profile. Proper preparation, standardized imaging protocols, and structured BI-RADS reporting significantly influence diagnostic accuracy.
Safety screening and quality-controlled image acquisition remain central to reliable breast imaging outcomes.
Images Diagnostic Center operates across Kuwait in:
For more information or to book your appointment, please contact our team. We are dedicated to providing the highest standards of care at Images Diagnostic Center, your trusted partner for diagnostic excellence in Kuwait.